You might feel fine. You might look fine. But inside, your liver could be fighting a silent battle that, if left unchecked, changes your life forever.
Fatty liver disease, previously known as Non-alcoholic Fatty Liver Disease (NAFLD) and recently renamed Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD), is a silent epidemic. It affects a massive portion of the world’s population, often without any noticeable symptoms until the damage is advanced.
The American Liver Foundation estimates that around 24% of the adults in the US have a fatty liver – most of them being unaware that they have it, which is why you should regularly consult your doctor, especially if you are considered at risk (overweight, family history, etc.)
I know this panic firsthand. I was diagnosed at 30 years old, when I was already starting to show signs (that I couldn’t understand at that time). But here is the good news: I managed to reverse this condition completely and anybody can do it too.
In this guide, we will look at what MASLD is, who is actually at risk (it’s not just people with obesity!), and the exact steps I took to heal it, backed by science and my own experience.
What is Non-Alcoholic Fatty Liver Disease (aka MASLD)?
Fatty liver disease, or MASLD, is exactly what it sounds like: a condition characterized by the accumulation of excess fat in liver cells. It is termed “non-alcoholic” because it isn’t caused by heavy alcohol use, though the damage looks very similar.
It’s also the most common form of chronic liver disease in the developed world, unfortunately.
When too much fat is stored in liver cells (as these amounts will grow if you’re not taking measures), it can cause inflammation and damage, leading to scarring (fibrosis), which can progress to cirrhosis or liver failure if not addressed.
The condition was traditionally known as NAFLD but has been reclassified to MASLD to emphasize its association with metabolic dysfunction, including obesity, type 2 diabetes, hyperlipidemia (high levels of fat in the blood), and hypertension.
This reclassification also highlights that the disease can affect individuals who are not obese, focusing attention on the broader metabolic factors involved.
Who is at Risk of Developing a Fatty Liver?
The risk factors for MASLD are closely linked to lifestyle and metabolic health issues. I would go as far as saying that anybody can get a fatty liver disease – it’s best to consider this and take proactive measures instead of the other way around.
Still, there are key groups that are at a higher risk of developing this condition:
- Obese individuals: Excess body fat, especially around the abdomen, increases the risk of developing MASLD, so people who are overweight (and above) are at a higher risk.
- People with Type 2 Diabetes: High blood sugar levels associated with type 2 diabetes can contribute to the accumulation of fat in the liver.
- Those with High Cholesterol or Triglycerides: An imbalance of blood lipids can lead to fat buildup in the liver.
- People with Hypertension: High blood pressure is often found in individuals with MASLD, suggesting a link between the two conditions.
- Genetic Factors: There’s a genetic predisposition to MASLD; individuals with a family history of the disease are at higher risk.
- Age and Gender: Although MASLD can affect individuals of any age, it is more common in those over 50. Men are also at a higher risk compared to women, though postmenopausal women’s risk increases.
As you can see, these risk factors do cover a pretty large amount of people. Understanding them, though, is important for early detection and prevention of MASLD.
It’s best to look for signs (or have these risk factors in mind) and make the required lifestyle adjustments, to significantly reduce the risk of developing a fatty liver disease.
The Danger of “Lean” Fatty Liver
There is a specific category of patients that have higher chances of getting a very late diagnostic: those with “Lean MASLD.”
These are individuals who have a normal Body Mass Index (BMI) and look thin but suffer from metabolic problems on the inside. Roughly 10% to 20% of people with fatty liver disease are not obese, but still have a diet high in processed sugar and saturated fats.
Their metabolism is fast and helps them look skinny, but the liver can still be drowning in fat. So unfortunately, even skinny people are at risk (although much lower).
The best way to know is by visiting a doctor. However, you can also take a look at these five warning signs that you might have MASLD.
Stages and Symptoms
The progression of MASLD occurs in stages, each with varying symptoms and implications for liver health.
While the fatty liver disease itself only has three stages (or grades) – afterwards becoming different conditions, basically, I want to group them all below for a better bigger picture.
IMPORTANT: Not all people go through all these stages – and not all of them go through them at the same pace. Some might live forever with “just” a fatty liver even without taking measures – although the risk of it getting worse is too big to be ignored.
1. Simple Steatosis (aka fatty liver)
This initial stage is characterized by the accumulation of fat in the liver, without significant inflammation or damage.
Most individuals at this stage experience no symptoms and may remain unaware of the condition unless detected through imaging tests or blood work.
This is what it’s normally called “fatty liver disease” and it’s divided into three stages. I wrote more in-depth on this matter here.
2. Metabolic Dysfunction-Associated Steatohepatitis (MASH)
Formerly known as NASH, this is where the situation gets serious and sees a subset of MASLD patients progressing to it. This is where liver fat accumulation is accompanied by inflammation and liver cell damage.
Symptoms may still be minimal or non-existent, but the risk of progressing to more severe liver damage is increased.
I recommend reading about the five warning signs that you might have a fatty liver. It’s always a good idea to catch it early and make the required changes in your life ASAP.
3. Fibrosis
Repeated or persistent inflammation can lead to the formation of scar tissue in the liver (fibrosis).
While still potentially reversible, fibrosis begins to stiffen the liver and affect its function.
4. Cirrhosis
The most advanced stage, cirrhosis, occurs when scar tissue extensively replaces healthy liver tissue, impairing liver function.
Symptoms become more pronounced and may include jaundice (yellowing of the skin and eyes), swelling in the legs and abdomen, and confusion.
Cirrhosis significantly increases the risk of liver failure and liver cancer.
It’s important to note that many individuals with MASLD do not progress beyond the early stages, and significant liver damage can be prevented with early detection and lifestyle modifications.
How is Fatty Liver Diagnosed?
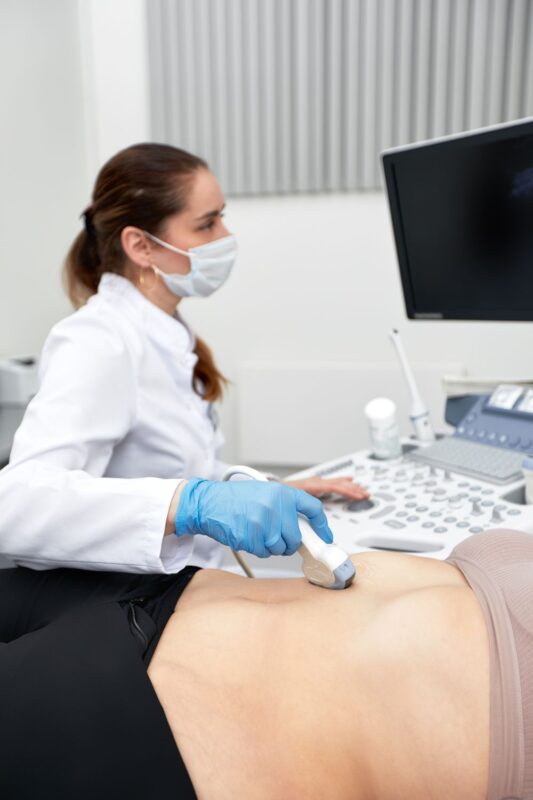
Diagnosing MASLD involves a combination of medical history, physical examination, blood tests, imaging studies, and sometimes liver biopsy.
But the easiest way of diagnosing it is through an ultrasound or CT Scan.
Blood test results can be deceptive and there are no perfect blood tests for MASLD. While elevated liver enzymes (ALT and AST) can indicate problems, many people have normal enzymes despite having the disease.
I am the perfect example of this: I had completely normal blood test results, yet an ultrasound revealed I had a fatty liver, which was later confirmed by a fibro scan.
The Best Diagnostic Tools
- Ultrasound or CT Scan: This is the most common way to “see” the fat. It is non-invasive and effective for diagnosis.
- FibroScan: This is a specialized ultrasound that measures liver stiffness (fibrosis) and fat content. It is incredibly useful for determining the stage of the disease.
- Biopsy: In rare cases, a doctor may need to take a tiny tissue sample to confirm the severity of inflammation, though this is becoming less common thanks to improved imaging technology.
Regular check-ups and monitoring are very important, especially for individuals at high risk of developing the disease.
Questions to Ask Your Healthcare Provider After Being Diagnosed
I know from personal experience how difficult and overwhelming it is to receive this diagnosis. I was 30 when I was diagnosed and when I got home, I started crying.
But after the initial round of crying is done, it’s time to actually get your life back on track. Reversing this condition is doable – I did it, and many people I talked and helped over the years did it too (many even without my help).
Being prepared with questions for your healthcare provider can help you understand your condition and the steps you can take to manage it effectively. Here are some essential questions to ask:
- What stage is my fatty liver disease at?
- What lifestyle changes should I prioritize to manage my condition? Specific advice on diet, exercise, and weight loss can provide a clear path forward.
- Are there any medications I should take or avoid? Knowing how your current medications or potential prescriptions can affect your liver health is crucial.
- How often should I have my liver function tested? Regular monitoring can help track the progression of the disease and the effectiveness of your management plan.
What is the Treatment for Fatty Liver Disease?

For a long time, the answer was simply “diet and exercise.” While that remains the foundation and the best way to tackle this situation, the medical landscape has changed lately.
In early 2024, the FDA approved Resmetirom (Rezdiffra) specifically for adults with MASH who have moderate to advanced liver scarring.
For those with type 2 diabetes or obesity, doctors may also prescribe GLP-1 agonists (like Semaglutide) which have shown promise in reducing liver fat indirectly through weight loss – with Wegovy now being FDA-approved as well for MASH patients.
Regardless of medication, though, you cannot fix a lifestyle disease without fixing your lifestyle. To cure my fatty liver, I had to completely overhaul my daily habits.
Here are the key strategies I used and worked well:
- Lifestyle Modifications: The most important part of fatty liver disease management, lifestyle changes aim to reduce liver fat, inflammation, and the risk of fibrosis. This includes:
- Weight Loss: Losing as little as 10% of body weight can significantly reduce liver fat. This is best achieved through a combination of diet and exercise – but don’t stop until you reach a good BMI (body mass index).
- Healthy Diet: A diet rich in vegetables, whole grains, fruits and lean proteins can help manage MASLD. Reducing intake of saturated fats, sugars, processed foods and refined carbohydrates is recommended.
- Physical Activity: Regular exercise, even without weight loss, can reduce liver fat. Aim for at least 150 minutes of moderate-intensity activity per week, like running or cycling.
- Control of Metabolic Risks: Managing diabetes, high blood pressure, and abnormal lipid levels is crucial. This may involve medications prescribed by a healthcare provider, along with dietary and lifestyle changes.
- NO Alcohol: Even though MASLD is not caused by alcohol, drinking can exacerbate liver damage. Avoiding alcohol is the only way to go, and not as difficult to achieve as you might think.
- Regular Monitoring: Periodic follow-up with healthcare providers to monitor liver health and the effectiveness of treatment interventions.
I have an in-depth guide for those who have just been diagnosed with a fatty liver. It covers all the steps that you must follow and lists them in order, so you’re not overwhelmed anymore.
Read my article here (it’s free!): Just Diagnosed with Fatty Liver? Here Is what to Do.
What to Eat vs. What to Avoid
Diet is the biggest lever you can pull. Here is a quick breakdown of what your plate should look like to reverse MASLD – but recommend going with my in-depth article here to get the big picture.
| Eat This | Avoid This |
| Cruciferous Vegetables: Broccoli, Brussels sprouts, and cauliflower contain compounds that help liver enzymes. | Added Sugars: High Fructose Corn Syrup is the enemy #1. It goes straight to the liver to be turned into fat, but all added sugars should be eliminated from your diet. |
| Coffee: Believe it or not, black coffee is shown to lower liver stiffness and reduce inflammation. | Refined Carbs: White bread, pasta, pastries, and anything with refined carbs spike insulin, which triggers fat storage. |
| Fatty Fish: Wild salmon and sardines are high in Omega-3s, which reduce liver fat. | Alcohol: Zero is the goal. Non-negotiable! |
| Healthy Fats: Extra virgin olive oil, avocados, and walnuts. | Red & Processed Meats: Limit beef, pork, and deli meats which are high in saturated fats. |
Role of Supplements in Managing MASLD
While lifestyle modifications remain the most important thing one can do to reverse fatty liver disease, there are some supplements that at least some experts consider to be helpful.
While these alone won’t cure your condition, they might help your body manage it better and recover faster.
There’s little medical proof for that at the moment, but generally, these supplements are considered safe and, worst case scenario, they will have no effect.
The main supplement is milk thistle, which is a natural extract used from ancient times – and the best known fatty liver supplement.
Other supplements include various multivitamins, especially vitamin E (read about the best multivitamin for fatty liver here), magnesium supplements, and also Omega-3 fatty acids.
Despite the potential benefits, it’s crucial to approach supplementation with caution, and always consult with a healthcare provider before taking anything.
How Can Fatty Liver Disease Be Prevented?
Preventing MASLD basically involves addressing the risk factors that lead to its development. Here are effective prevention strategies:
- Maintain a Healthy Weight: Achieving and maintaining a healthy weight through diet and exercise is one of the most effective ways to prevent MASLD.
- Eat a Balanced Diet: Focus on a diet that includes plenty of vegetables, whole grains, fruits and healthy fats. Avoid excessive amounts of sugar and saturated fats, but also processed foods.
- Exercise Regularly: Engaging in regular physical activity helps control weight and reduce liver fat.
- Manage Blood Sugar: Keeping blood sugar levels within a healthy range can prevent the development of type 2 diabetes, a risk factor for MASLD.
- Keep Cholesterol and Triglycerides in Check: Managing these blood lipids can help prevent liver fat accumulation.
- Limit Alcohol Consumption: Reducing alcohol intake can decrease the risk of liver damage. Ideally, stop drinking alcohol completely.
- Regular Health Check-ups: Regular monitoring of health markers can help identify risk factors early and prevent the development of MASLD.
Have in mind though, that sometimes genetics play an important role here and there’s not much some people can do.
I have talked with quite a few people who lived a healthy life, ate clean food and were in good physical shape… but still developed a fatty liver.
Sometimes, you just have to deal with whatever life has in plan for you, no matter how much you strive.
But still, what I tell these people is this: Even though it’s discouraging to have a fatty liver despite living a healthy life, it would be MUCH worse if you weren’t.
Pin this for later:


Final Thoughts
When it comes to managing MASLD aka fatty liver disease, a one-size-fits-all approach doesn’t really work.
The condition’s complexity and its potential connections to other health factors and diseases you might have mean that its management and treatment are usually tailored to the individual.
The principles remain the same though, with the main change required after being diagnosed being that of the diet, followed by lifestyle changes that include exercising and potentially taking some supplements to speed up the process.
The best news is that fatty liver disease is a reversible condition. I managed to reverse my fatty liver in 1.5 years after my original diagnosis.
I also saw tens of people, over the years, reversing their condition – we’re talking about it on the Facebook Group (which is private, so I invite you to join it to discuss with other people in your situation.
Disclaimer: I am not a doctor. This article is based on my research and personal experience. Always consult with a medical professional for advice tailored to your specific situation.
Sources & Resources: NHS, NIH, Wikipedia, Hopkins Medicine.

I was diagnosed with fatty liver in 2014 and successfully reversed it by mid-2015 using a natural diet and lifestyle changes. Since then, I’ve dedicated over a decade to researching this condition and helping others navigate their own recovery. I am the author of ‘From Fatty Liver to Healthy Liver’ and the founder of this community. My goal is to translate complex medical studies into practical, real-world advice that actually works, combined with my personal experience on the matter.